Enabling High-Touch Care at Scale
I redefined how care delivery works at Honor by addressing the structural platform gaps limiting consistency and scale, redesigning how work is generated and routed across the platform.
My journeyResearch > System mapping > Problem reframe > Collaborative vision > Driving two dual workstreams > Converged MVP
My rolePrinciple product designer leading end-end design, strategy & research.
Team structure2 designers, 6 engineers, 2 data scientists, 1 researcher, 3 Care Team leaders, Product Director & CPO
Timeline6+ months
Impact this made
Client retention12% ↑
Increase in client retention over a three month period
Efficiency22% ↑
488hr/wk via automation, prioritization of work & reduced agency coordination
Care Pro Preparedness8% ↑
Increase in visit satisfaction and client retention
OrganizationNew platform pod & framework
Evolved client manager role & KPIs
Problem space
Honor is the world’s largest home care network, providing nearly 1 million hours of care weekly through its advanced care platform. In 2021, Honor acquired Home Instead, the largest home health care franchise network in the U.S.
Post-acquisition, some agencies were hesitant to transfer their operations to Honor due to their deep client relationships, causing inefficiencies as they continued to co-manage operations. This remained a challenging space that Honor continuously tried to solve for and in late 2023 it became a main focus area for the product development team. I came in as the principal designer for this space and was tasked with spearheading efforts across the system to significantly reduce manual coordination in order to effectively integrate more agencies into the platform.
Honor's user ecosystem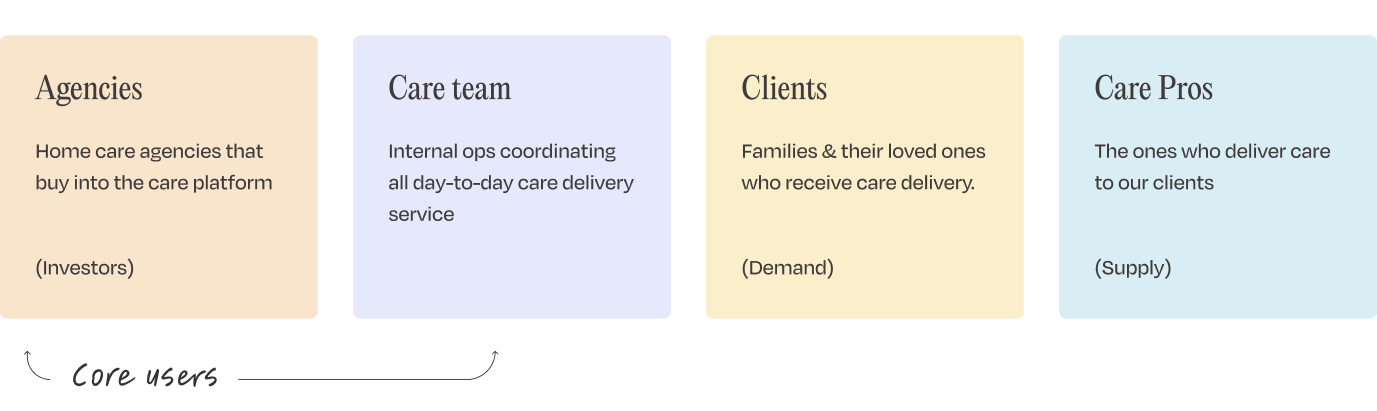
DiscoveryGetting to the root
Before proposing solutions, I revisited past feature launches and process changes to understand what had been attempted and why it had not fully worked.
I then led 12+ interviews and shadow sessions across care operations and agency partners to see how coordination actually functioned in practice. In parallel, I partnered with data to quantify the time spent in manual coordination and where it was accumulating across the system.
This gave me the clarity to move beyond surface inefficiencies and define the structural problem we needed to solve.
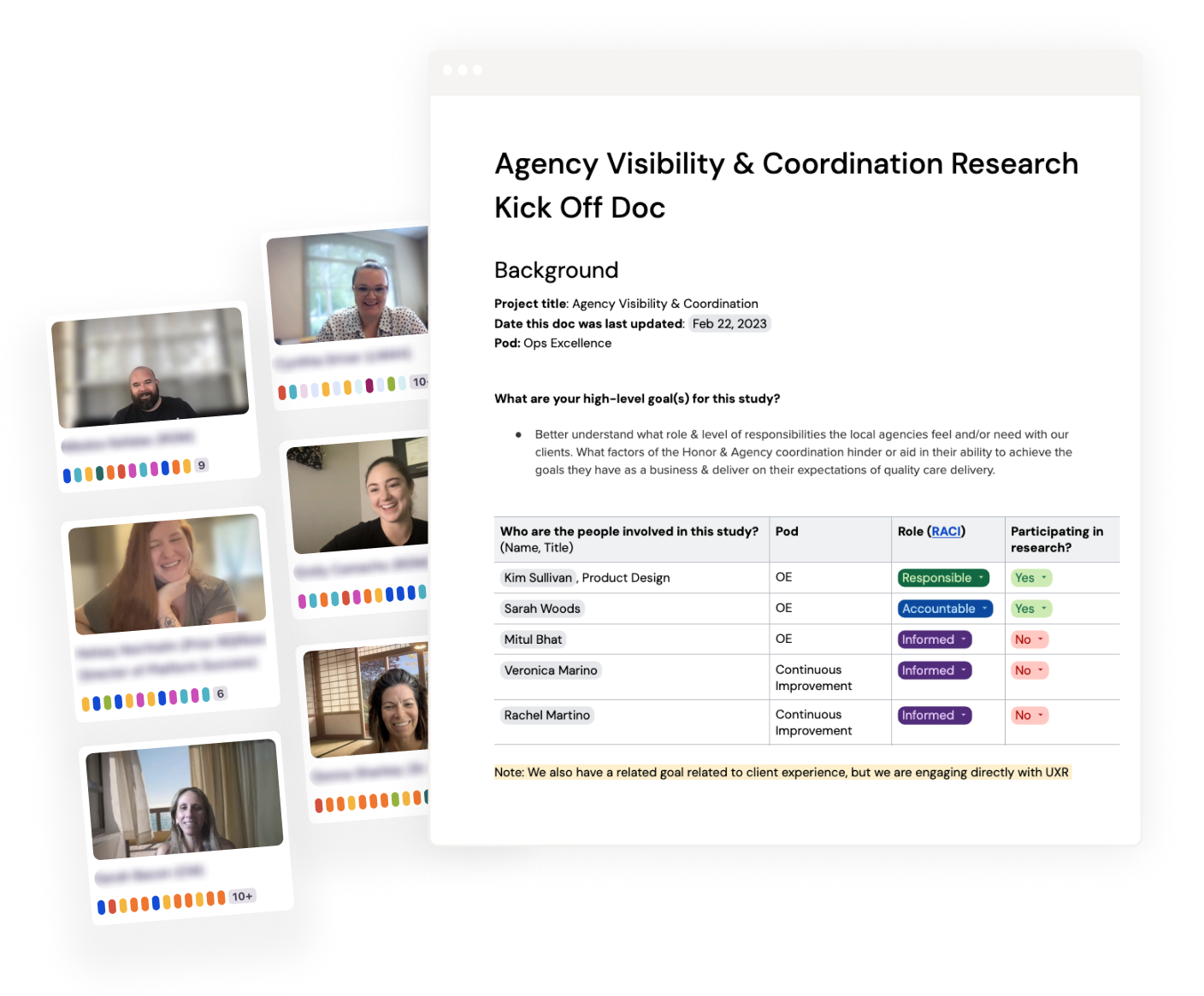
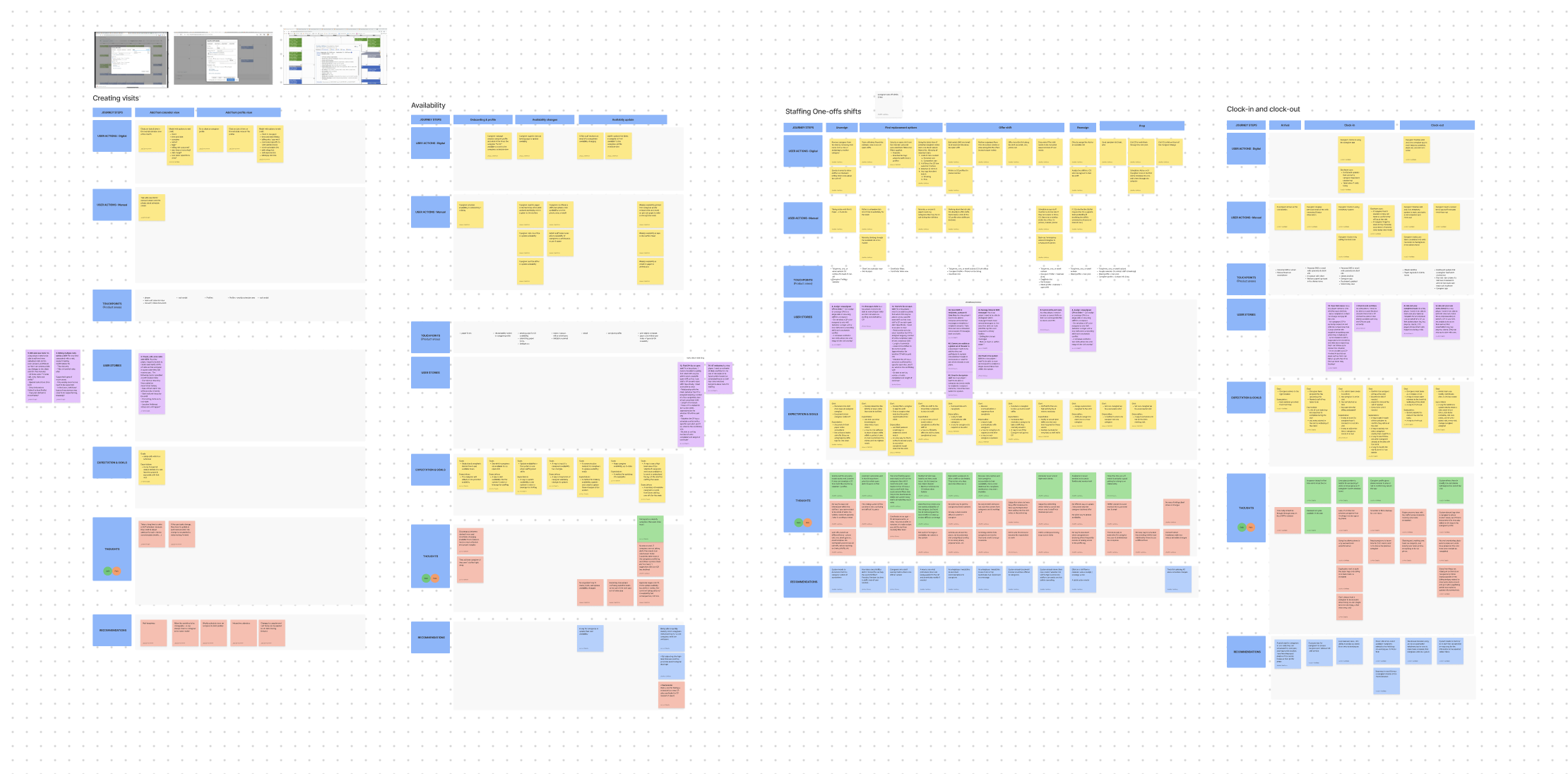
What we did not fully understand was how clients experienced working with two operating partners, or how that confusion affected retention and growth.
I partnered with our Head of UXR, Rose Kue, to lead a deep dive into the client service experience. It was the first time we had examined this relationship end to end, and it became a critical unlock in my discovery.
What we learned fundamentally reshaped how I framed the problem for leadership.
I think that this whole company should be rearranged to make it more personal and more safe for these elderly people.
— Family member of client
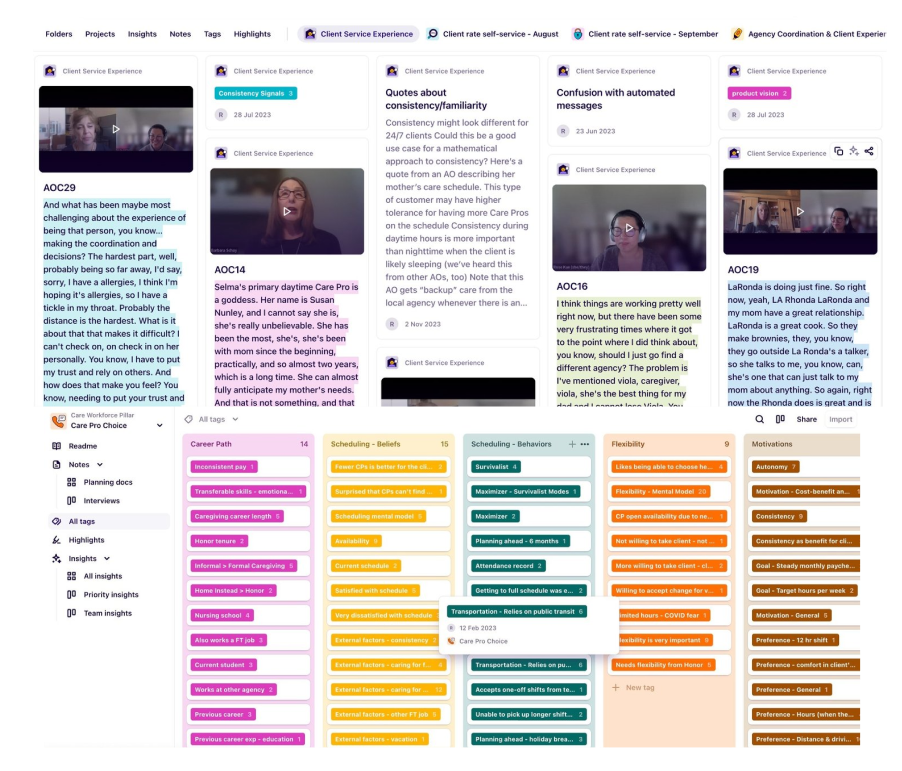
Snippet of our Client Service Experience synthesis
The pivotReframing the problem
Our study surfaced a critical gap. Many clients did not fully understand the Honor and Home Instead partnership, and some felt care had become less personal and less high-touch. When I synthesized the research and data, three structural issues emerged:
Work was untraceable
~60% of the work was unable to be internally tracked or visibleLack of prioritization
Our product is a “pick your own adventure” forcing teams to work reactivelyInconsistency in outcomes
Care team & agencies working differently, delivers inconsistent results.
Our real problem
Honor lacks product-driven orchestration of the customer experience and therefore cannot deliver an acceptable customer experience at our current scale.
CollaborationDefining the north star
Once we aligned on the real problem, the question became how to scale quality care without losing the high-touch experience agencies valued.
Past attempts in this space had not worked, and there was understandable skepticism about whether “white glove” service could exist inside a system-driven model. I partnered closely with my Product Director to define both the long-term vision and a pragmatic execution path forward.
Over several weeks, I facilitated focused working sessions with fellow principal designers to identify structural gaps in the platform that were contributing to service breakdowns. These sessions helped us move from abstract ambition to concrete system changes required to support proactive, consistent care delivery.


Images taken during my 2 day facilitated brainstorm session with other design leads
In parallel, I facilitated cross-functional workshops with care operations, engineering, data, product, and design to explore how the platform could shift from supporting manual coordination to driving proactive care delivery.
Those sessions helped us move from abstract ambition to concrete system changes. More importantly, they clarified our north star: shift the system from reactive support to proactive orchestration, with measurable improvements in client retention, operational efficiency, and care quality:
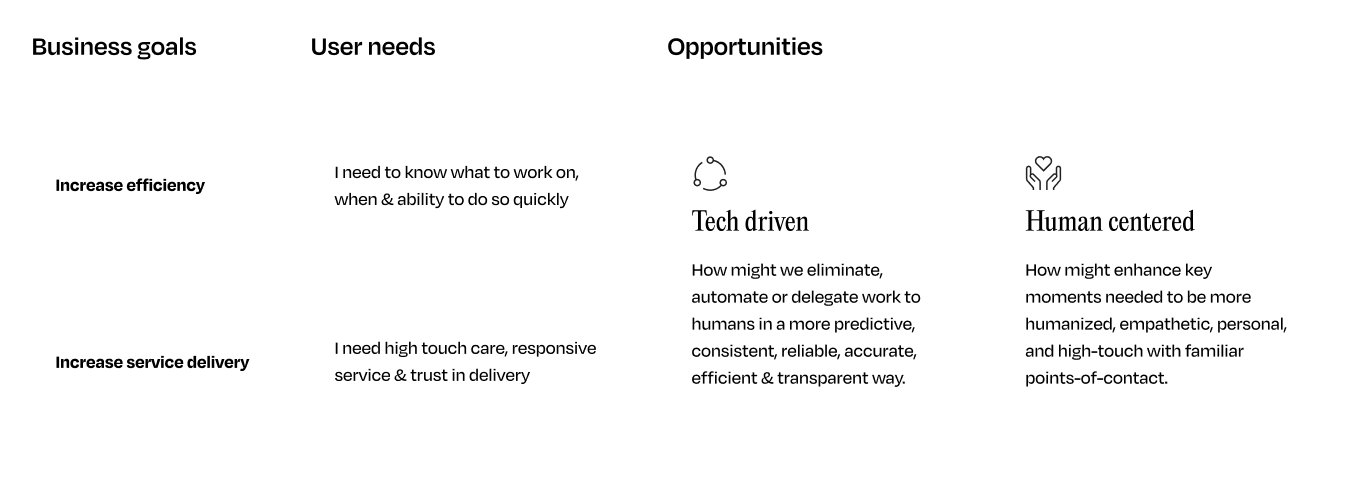
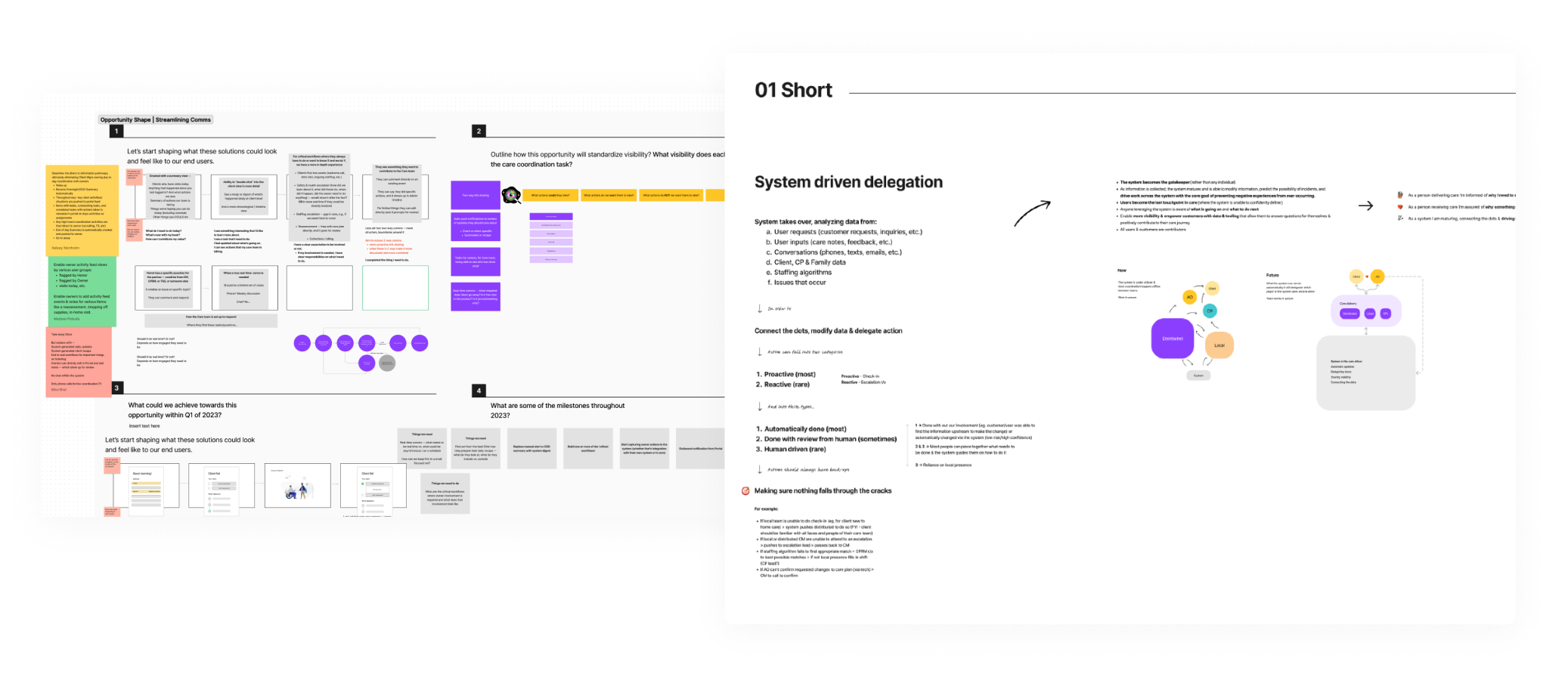
VisionArticulating the future of Honor
The vision was simple but transformative. The system, not humans, would orchestrate care.
Work would be generated, prioritized, and delegated intelligently. Low-touch tasks would be automated. High-touch moments would be surfaced with context and urgency. External partners would engage through structured workflows rather than ad hoc coordination.
By redesigning how responsibility flowed through the platform, we could scale high-quality care without scaling operational overhead at the same rate.
When the cost implications became concrete, the conversation shifted. The vision was no longer aspirational. It became a strategic investment.
Iteration & developmentDesigning the New System of Care
To make the vision real, I led two parallel workstreams that tested both the system itself and the human experience around it.
01 Building the proof of concept
The first track focused on validating the orchestration layer technically. I partnered closely with engineering to define the underlying data model that would power system-generated and prioritized work.
In parallel, I created high-level concepts to demonstrate how this framework could surface across both internal tools and external experiences. This gave the team (designs & engineers) something concrete to build against and allowed us to test the shift from reactive coordination to system-guided work.
02 Piloting High-Touch Care
At the same time, we needed to test the human side of the equation.
We launched a manual pilot that redefined the Client Manager role as the single point of contact for families, replacing the previous frontline team model. Instead of fragmented interactions, clients had one accountable relationship owner.
This pilot allowed us to evaluate whether clearer ownership and more structured engagement improved trust, satisfaction, and retention, while also revealing which workflows would need to be supported or automated by the system long term.
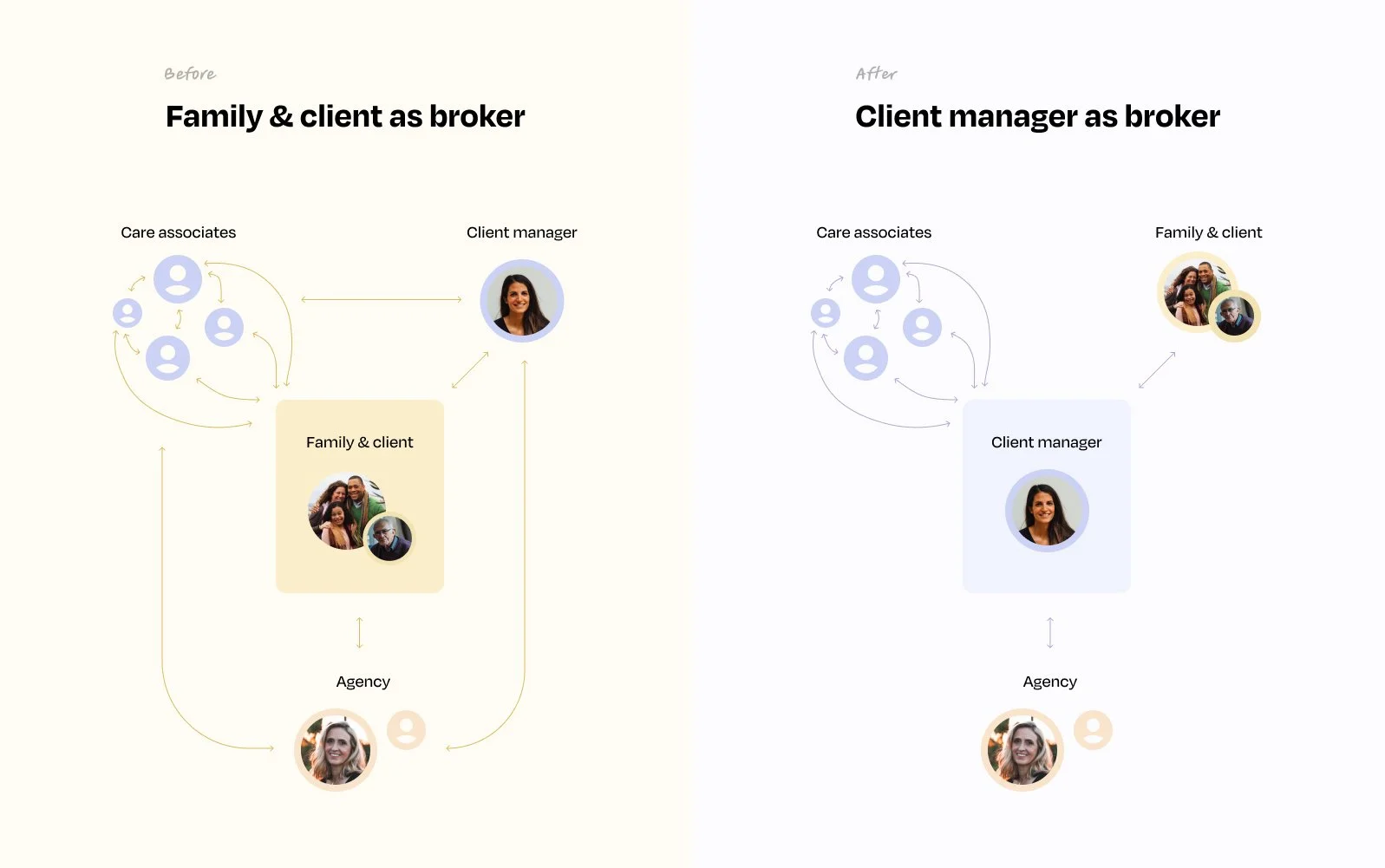
Applying these learnings
The pilot improved retention and clarified where high-touch care truly mattered.
Combining those insights with the orchestration framework, we prioritized the workflows most critical to scaling quality, especially pre- and post-visit moments and manual Care Pro preparation.
These became the foundation for our first system-driven workflows.
OutcomeFrom Coordination to Orchestration
This work fundamentally changed how responsibility moved through the platform. Instead of teams manually hunting for tasks and coordinating across dashboards, the system now drives and safeguards care delivery.
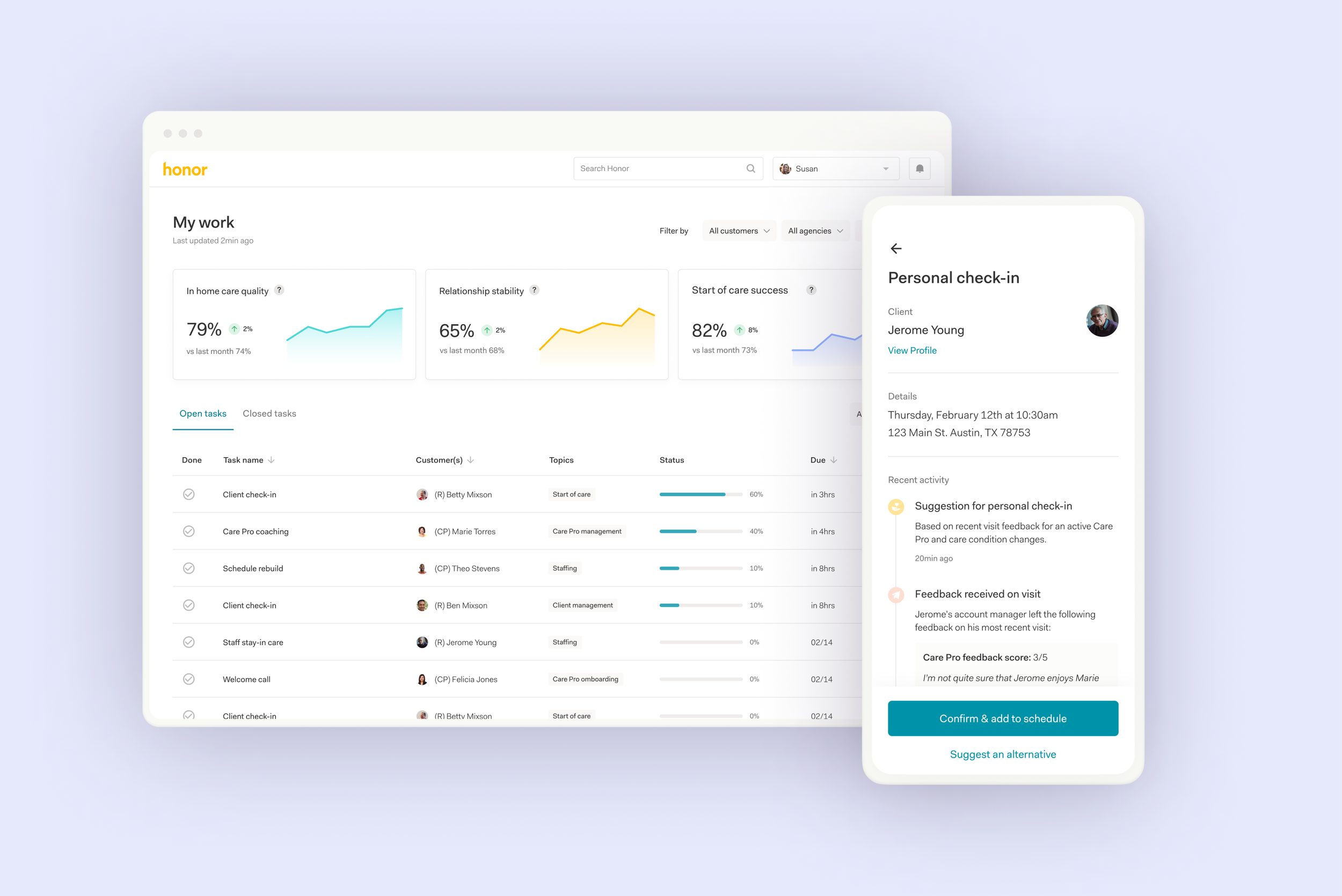
System-Prioritized Work
We introduced a centralized, dynamic work queue that generates and sequences tasks for each operational team member. This replaced five primary dashboards and eliminated fragmented coordination, allowing the system to determine what matters most while teams execute from a single, guided view.
Guided Workflow Completion
We transformed high-impact workflows, including pre- and post-visit moments and manual Care Pro preparation, into structured, trackable flows within the queue. By modularizing the contextual data required to complete them, we reduced navigation across the platform and created a scalable foundation for future automation.
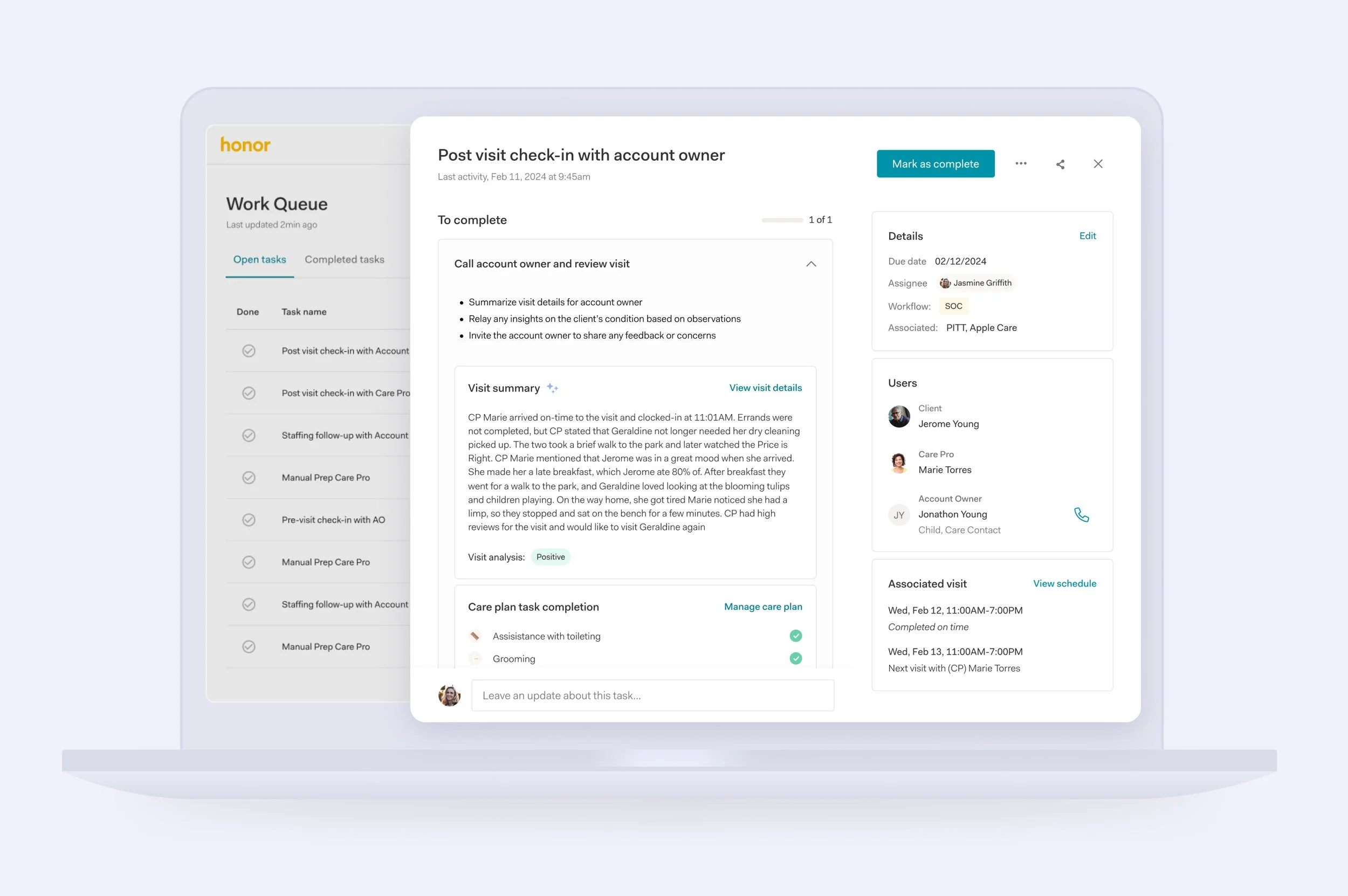
Self-Service With Safeguards
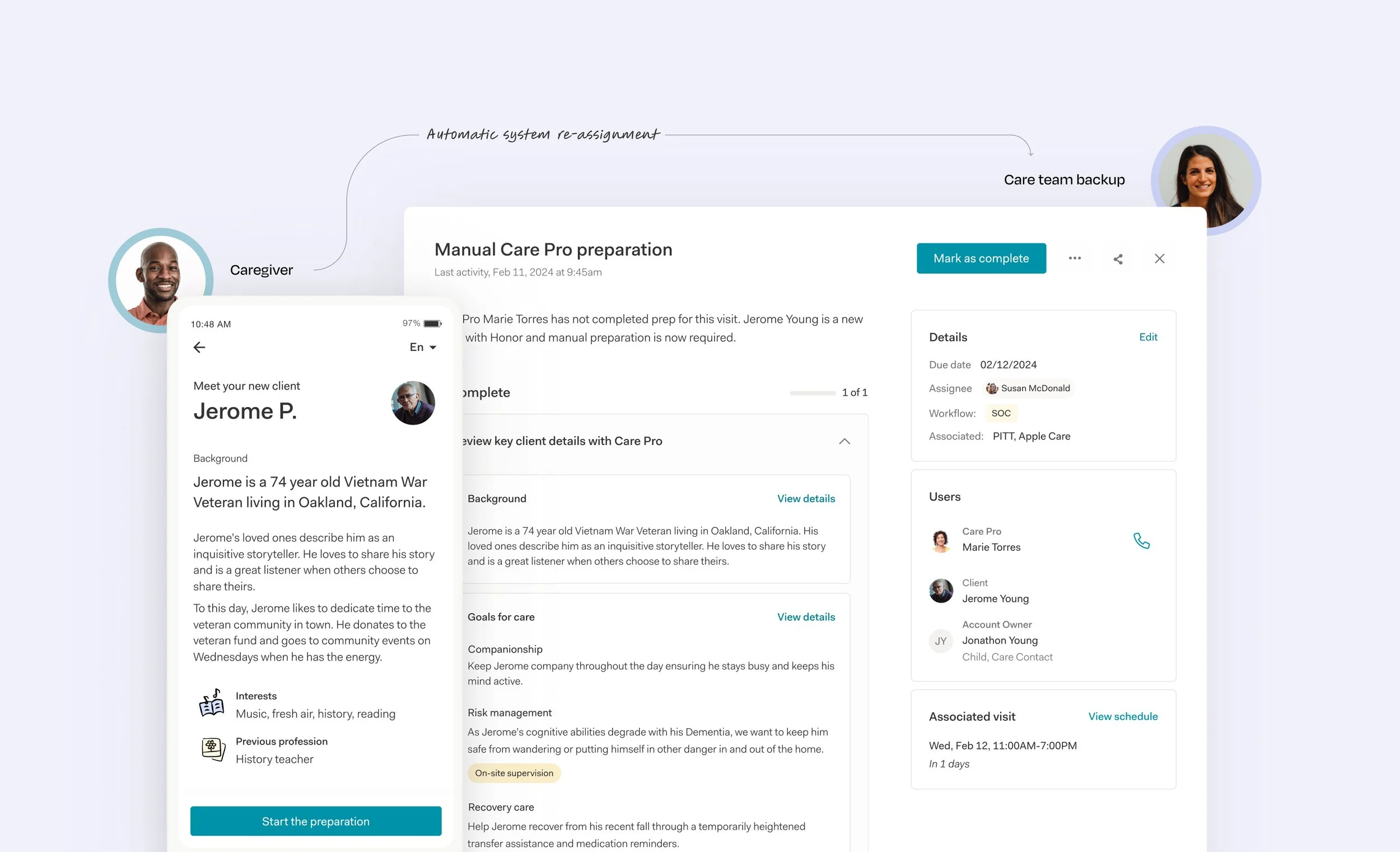
We redesigned caregiver visit preparation as our first external workflow under the new framework, reducing manual phone and text coordination while increasing preparedness. If key actions are not completed by their due date, the system automatically reassigns the work internally, ensuring quality does not silently fail.
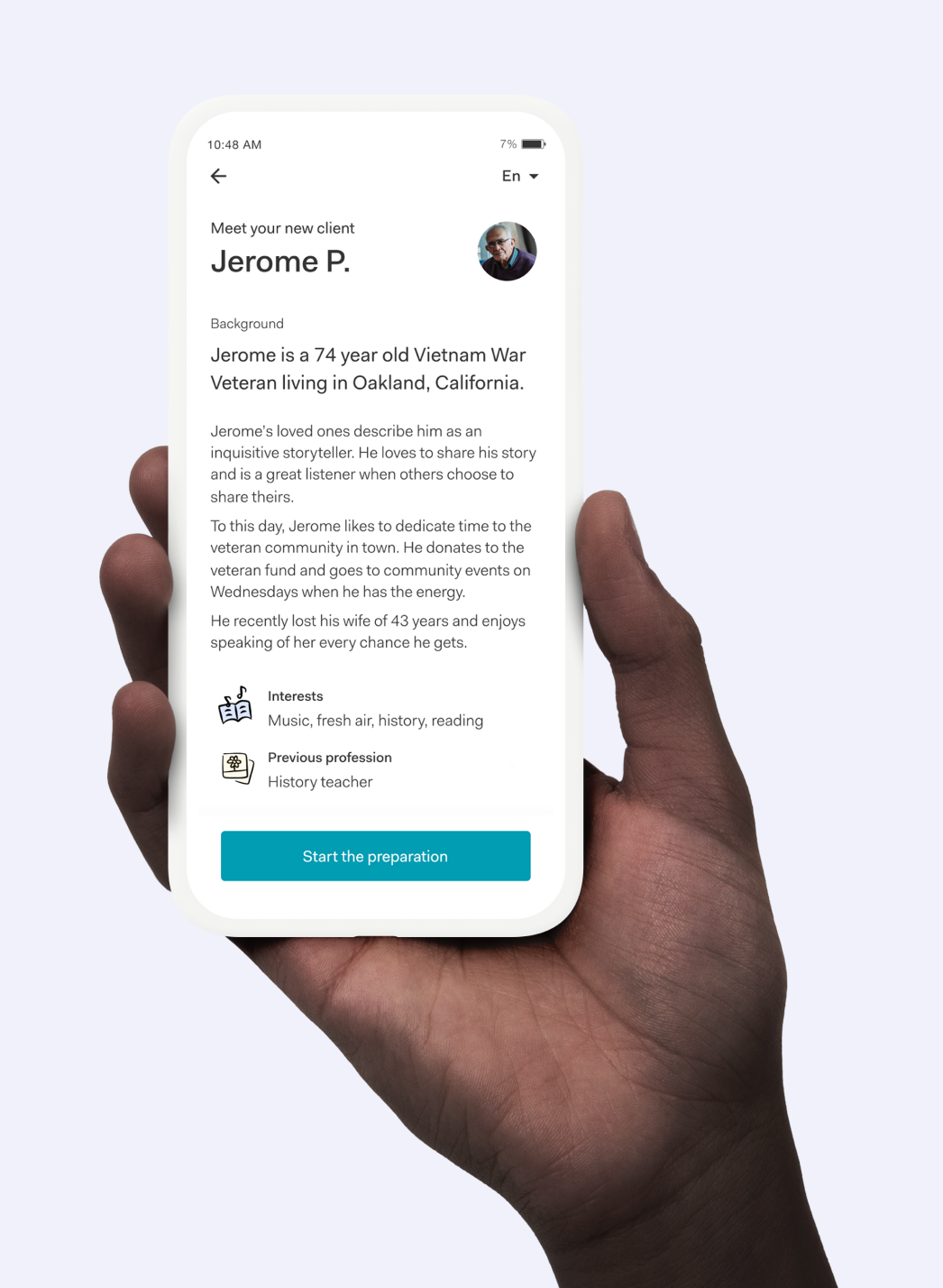
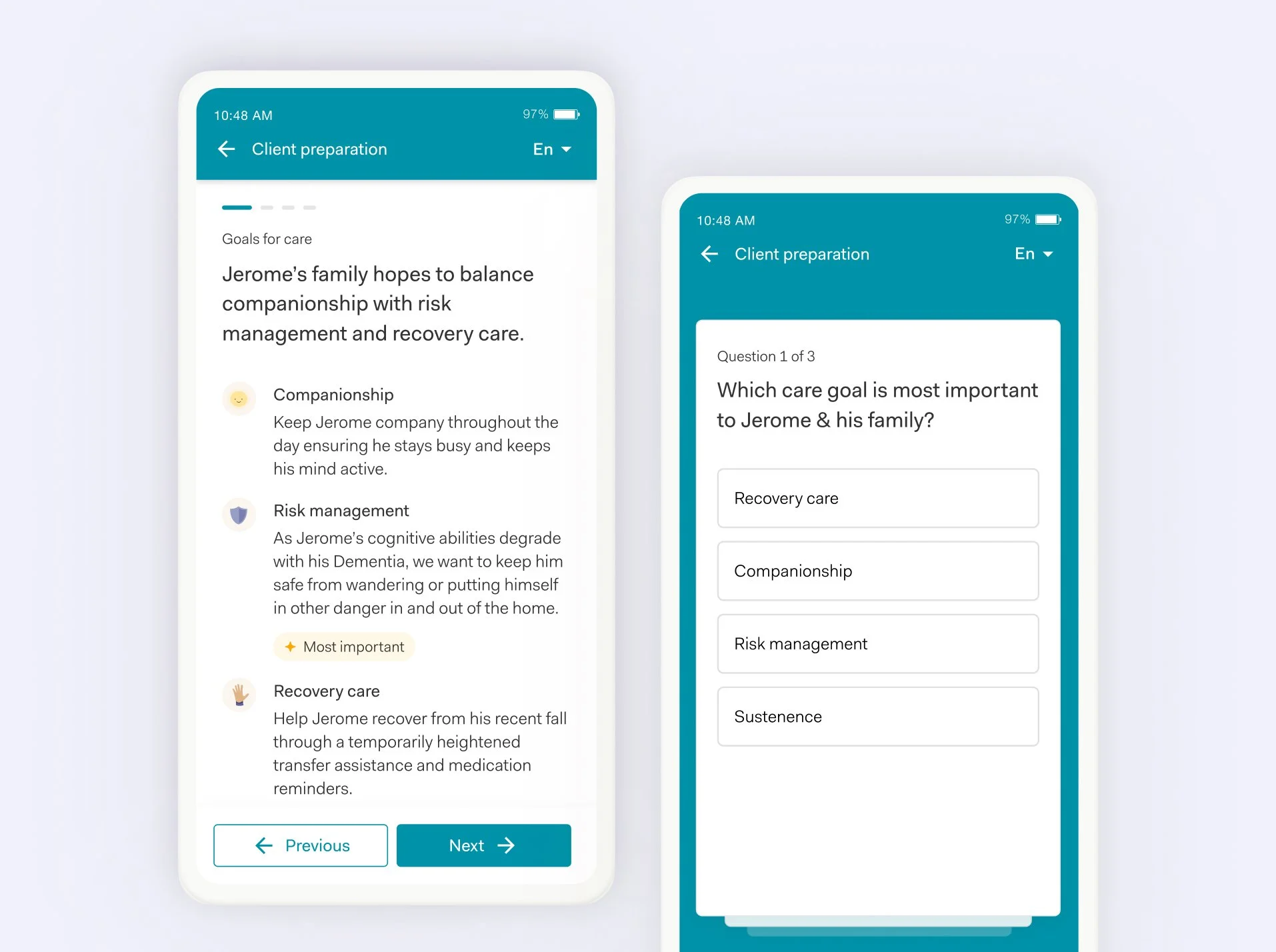
Built-In Safeguards
The system now detects when critical care steps are not completed and automatically reroutes the work internally. Instead of relying on manual follow-up, we built safeguards directly into the platform to ensure quality care is always delivered.